Introduction: Rising Concern Over Legionnaires' Disease in North Carolina
North Carolina is witnessing a worrisome surge in Legionnaires' disease cases, prompting urgent warnings from public health officials. According to the North Carolina Department of Health and Human Services (NCDHHS), there has been a more than 50% increase in reported cases of this severe respiratory illness from 2024 to 2025 [Source: Source]. This sharp uptick has raised alarms among medical professionals and state authorities, who are now urging both residents and healthcare providers to stay vigilant. Legionnaires’ disease, a potentially life-threatening form of pneumonia, is especially dangerous for certain high-risk groups. As the state investigates the underlying reasons for this rise, the focus is on spreading awareness, improving early detection, and reinforcing preventive measures to safeguard public health.
What is Legionnaires' Disease?
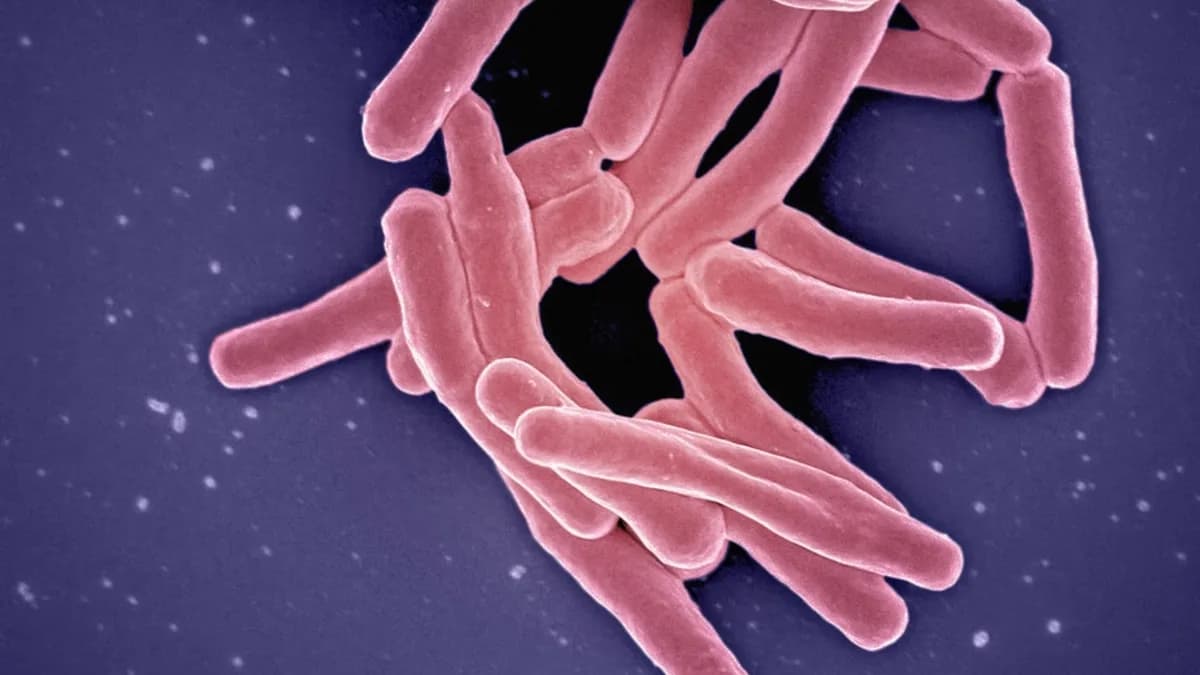
Legionnaires' disease is a serious lung infection caused by the Legionella bacteria. Unlike the common cold or flu, it can lead to severe pneumonia and, in some cases, prove fatal if not treated promptly. The illness was first identified in 1976 after an outbreak at an American Legion convention, which gave the disease its name.
Legionella bacteria thrive in freshwater environments but become a health risk when they multiply in man-made water systems. Common sources of infection include cooling towers used for air conditioning in large buildings, complex plumbing systems, decorative fountains, and hot tubs. People typically contract Legionnaires’ disease by inhaling tiny droplets of water (aerosols) containing the bacteria. It is important to note that it does not spread from person to person.
Symptoms often resemble other types of pneumonia and can include cough, shortness of breath, high fever, muscle aches, and headaches. The illness usually develops two to 10 days after exposure to the bacteria. While anyone can be infected, certain groups are more vulnerable: adults over 50, smokers, individuals with chronic lung disease, and those with weakened immune systems (such as transplant recipients or people with cancer). For these individuals, the risk of complications is significantly higher, underscoring the need for early recognition and intervention.
Why Are Cases Increasing in North Carolina?
The recent rise in Legionnaires' disease cases in North Carolina has prompted several questions about its underlying causes. Environmental and infrastructural factors play a substantial role. Many communities across the state rely on aging water systems, which can be more prone to corrosion and biofilm formation—conditions that allow Legionella bacteria to thrive. Additionally, North Carolina’s climate, with its warm and humid summers, can further encourage bacterial growth in stagnant water systems [Source: Source].
Another key factor is the increased awareness and vigilance surrounding Legionnaires’ disease. Improved diagnostic testing and stronger public health surveillance mean that cases are more likely to be identified and reported than in previous years. The NCDHHS has intensified efforts to monitor respiratory illnesses, leading to more accurate and timely detection of outbreaks [Source: Source]. This improved reporting may partially account for the higher numbers, as cases that historically went undiagnosed are now being recognized.
At the same time, population growth and urbanization contribute to more complex and extensive water systems in buildings, increasing the risk of contamination if maintenance falters. The convergence of these factors—aging infrastructure, environmental conditions, and heightened surveillance—appears to be driving the current spike in reported cases.
Public Health Response and Preventive Measures
In response to the surge in Legionnaires’ disease, North Carolina health officials have ramped up efforts to monitor and control potential outbreaks. The NCDHHS is working closely with local health departments, hospitals, and laboratories to track cases, investigate sources, and implement infection control measures [Source: Source]. Rapid identification of exposure sites is crucial for preventing further transmission, especially in facilities serving high-risk populations such as nursing homes and hospitals.
Building managers and business owners are being provided with updated guidance on how to maintain and disinfect water systems. Proper management of cooling towers, hot water tanks, and decorative fountains is critical to reducing the risk of Legionella growth. Regular cleaning, temperature control, and flushing of infrequently used water lines are among the recommended practices. The Centers for Disease Control and Prevention (CDC) also advises the development of water management programs for large or complex buildings.
For individuals, public health messages emphasize the importance of recognizing symptoms early and seeking prompt medical attention. Doctors have been alerted to consider Legionnaires’ disease when evaluating patients with pneumonia, particularly if they have risk factors or potential exposure to contaminated water sources. Quick diagnosis and treatment with antibiotics can significantly improve outcomes.
How Residents Can Protect Themselves
While much of the responsibility for preventing Legionnaires’ disease falls on institutions and building managers, residents can also take practical steps to reduce their risk. One of the simplest precautions is to avoid exposure to stagnant or poorly maintained water sources in homes and public places. Homeowners should ensure that water heaters are set to a temperature high enough to kill bacteria (generally at least 120°F/49°C) and run faucets and showers regularly to prevent water from sitting in pipes too long.
Individuals with weakened immune systems or chronic lung conditions should be especially cautious when using hot tubs, public showers, or decorative fountains. If such facilities appear dirty or poorly maintained, it is best to avoid them.
Early diagnosis is crucial. Anyone experiencing persistent cough, fever, muscle aches, or shortness of breath—especially with a history of recent travel, hospital stay, or exposure to large building water systems—should seek medical attention promptly. Informing healthcare providers about potential exposures can help ensure timely testing and treatment, reducing the risk of severe complications.
Conclusion: Staying Informed and Vigilant Against Legionnaires' Disease
The recent increase in Legionnaires’ disease cases in North Carolina highlights the continuing challenge posed by waterborne illnesses. As the state confronts more than a 50% rise in cases, public health officials are urging residents and healthcare providers to stay informed, practice preventive measures, and report any suspected outbreaks swiftly [Source: Source]. Community cooperation is essential—whether it’s building managers ensuring safe water systems or individuals recognizing symptoms and seeking care.
Ongoing efforts by the NCDHHS and local partners aim to strengthen surveillance, improve rapid response, and educate the public. With vigilance and proactive action, North Carolina hopes to curb this rising trend and protect its most vulnerable residents from the serious risks posed by Legionnaires’ disease.